New Manitoba Technology Could Transform Breast Cancer Detection
The field of breast cancer diagnostics may be approaching a significant shift, with early-stage research emerging from Manitoba, Canada. A collaborative team from the University of Manitoba and affiliated medical institutions has developed a novel imaging approach that shows strong potential for improving detection accuracy—particularly in patients with dense breast tissue, where conventional mammography is less effective.
Findings from early clinical studies suggest the technology could address a long-standing limitation in screening and potentially improve early diagnosis rates.
The Ongoing Challenge in Breast Cancer Screening
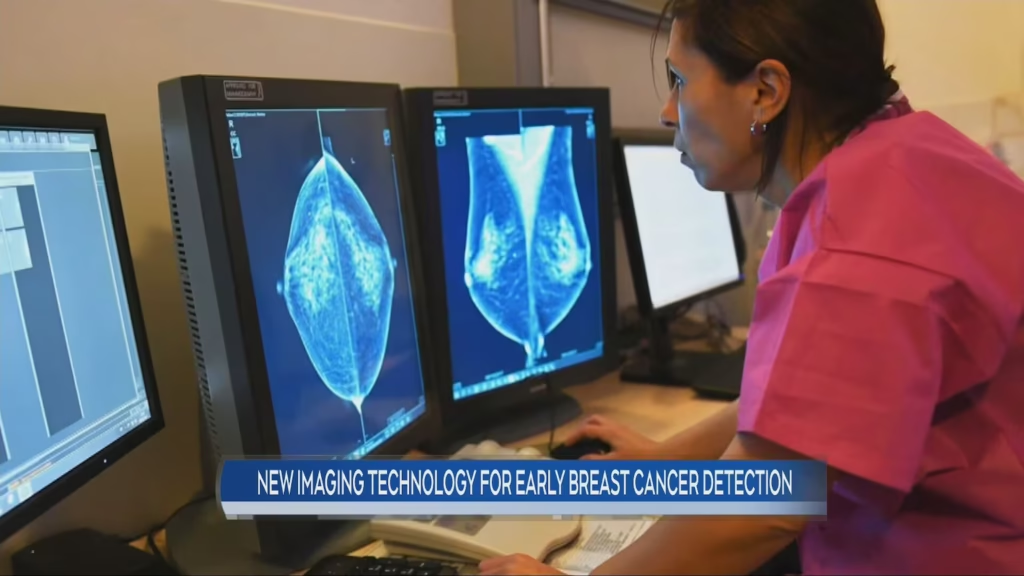
Mammography remains the standard tool for breast cancer screening, but it has well-recognized limitations. One of the most significant is its reduced sensitivity in dense breast tissue, which is present in nearly half of all women.
On a mammogram, both dense tissue and tumors appear white, making it more difficult to distinguish abnormalities. Clinical data shows that sensitivity can drop substantially in these cases, increasing the risk of missed or delayed diagnoses.
While supplemental tools such as ultrasound and MRI can improve detection, each has drawbacks:
- Ultrasound can produce higher false-positive rates and depends heavily on operator skill
- MRI offers high sensitivity but is costly, time-intensive, and often requires contrast agents
The Manitoba research team aimed to develop a method that bridges these gaps by capturing additional biological information beyond structural imaging alone.
How the Manitoba Imaging System Works
The new technology is based on a hybrid photoacoustic–ultrasound imaging system, which combines laser stimulation with conventional ultrasound detection.
Unlike mammography, which relies primarily on differences in tissue density, this system detects functional changes in tissue—particularly blood oxygenation and microvascular activity associated with tumor growth.
Photoacoustic Imaging Explained
The process works through a sequence of physical interactions:
- A short-pulse laser is directed into breast tissue
- Light is absorbed by hemoglobin in blood vessels
- This absorption generates a rapid, localized thermal expansion
- The expansion produces ultrasonic waves
- These waves are captured and reconstructed into detailed images
The Manitoba team’s key advancement lies in optimizing both the laser source and detector configuration for breast tissue, enabling faster and more practical clinical imaging.
According to researchers, the system can produce near real-time results in under three minutes without requiring invasive procedures or contrast agents.
Early Clinical Findings
In preliminary trials involving more than 200 patients at Winnipeg’s Health Sciences Centre, the system demonstrated promising performance metrics compared with conventional imaging approaches.
Reported outcomes include:
- High sensitivity for detecting malignant lesions in dense breast tissue
- No use of ionizing radiation
- No need for injected contrast agents
- Combined structural and functional imaging in a single scan
Researchers emphasize that these results are early-stage and require validation in larger, multi-center studies before clinical adoption.
Dr. Michael Le, one of the project’s lead physicists, described the approach as a shift toward functional imaging, noting that tumor metabolism may provide clearer diagnostic signals than structure alone.
Potential Impact on Patients and Health Systems
If validated at scale, the technology could have several important implications for both patients and healthcare systems.
For patients:
- Fewer false-positive results and reduced recall rates
- Earlier detection in cases where mammography is limited
- Lower exposure to unnecessary invasive follow-up procedures
For healthcare systems:
- Reduced reliance on expensive imaging modalities such as MRI
- Faster scan times compared to current advanced imaging tools
- Improved accessibility in rural and underserved communities
The portability of the system is also notable, with researchers indicating it could eventually be deployed in mobile screening units.
Dr. Priya Sharma, a breast surgeon involved in the trials, noted that the technology could eventually support targeted screening for high-risk populations, particularly women with dense breast tissue.
Technical and Clinical Challenges
Despite promising early data, several limitations remain.
Current technical constraints include:
- Reduced effectiveness in larger breast sizes due to light penetration limits
- Need for controlled lighting conditions during imaging
- Requirement for further optimization of hardware for broader clinical use
Additionally, the technology must undergo larger-scale clinical trials before regulatory approval can be considered.
A multi-center study involving approximately 1,500 patients is expected to begin in the coming years, followed by regulatory review through Health Canada and the U.S. FDA if results remain consistent.
Future Applications Beyond Breast Cancer
Researchers are also exploring broader applications of the platform. Because the system captures both structural and functional information, it may be adapted for:
- Thyroid nodule evaluation
- Skin cancer depth assessment
- Lymph node analysis during cancer staging
- Monitoring tumor response to treatment
Work is also underway to develop smaller, handheld versions for use in low-resource or remote healthcare settings.
A Step Forward in Diagnostic Imaging
Breast cancer remains one of the most commonly diagnosed cancers among women in Canada, and early detection continues to be the strongest predictor of survival.
While still in development, the Manitoba system represents a potential shift in how imaging technology approaches the problem—not just by improving image clarity, but by measuring biological activity associated with disease.
Further validation will determine whether it can move from promising prototype to clinical standard. For now, it stands as an example of how advances in hybrid imaging may reshape cancer detection in the years ahead.